SCIENCE
Vagus nerve - the heart and breathing
The Vagus Nerve (10th Cranial Nerve) is the longest and most important autonomic nerve bundle in the body. It is for instance the main information path between the brain and the gut. It has a number of branching nerves that go to the heart, lungs, voice box, stomach, ears, and other organs.
It monitors the condition of these organs and it is also considered a vital part of the immune system. Its most important ‘internal-organ’ role is to keep up homeostasis in the body. In everyday life, we know it mostly for its calming effect on stress and our ‘fight-or-flight’ responses. From this, it is known as the ‘rest-and-digest’ nerve.
Breathing, Heart Rate and the Vagus Nerve:
The vagus nerves are responsible for the lowering of the heart rate and in the lungs the vagus nerve causes bronchoconstriction and expansion to enable efficient oxygenation periodicity. When the autonomic nervous system is working normally, the vagus nerve is speeding up the heart rate during inhalation and decreases heart rate during exhalation.
This variation is critically important for determining oxygenation and in its ‘derived’ forms are currently used as the basis in all wearable sports- and health diagnostics involving heart rate. One traditional way to see this vagal tone is by measuring Heart Rate Variability (HRV) but for it to be accurate the measurement should be done for longer times and not by optical heart rate sensors which are inherently inaccurate.
Important parts of the vagus nerve:
The dorsal vagus nerve – which is the unmyelinated part of the vagus nerve sends which communicates with the viscera, especially to the intestines. This part of the vagus nerve is also responsible for extreme fear-reactions such as ‘freeze’ reactions and is overactivated in states of chronic fear.
The ventral vagus nerve is evolutionarily the newer part which is myelinated. Its extensions are mainly situated in the upper part of the body. It is considered responsible for many autonomic emotional- and human interaction functions.
The nucleus ambiguus – which gives rise to the branchial efferent motor fibers of the vagus nerve and preganglionic parasympathetic neurons that innervate the heart.
The solitary nucleus – which receives afferent taste information and primary afferents from visceral organs.
The spinal trigeminal nucleus – which receives information about deep/crude touch, pain, and temperature of the outer ear, the dura of the posterior cranial fossa and the mucosa of the larynx.
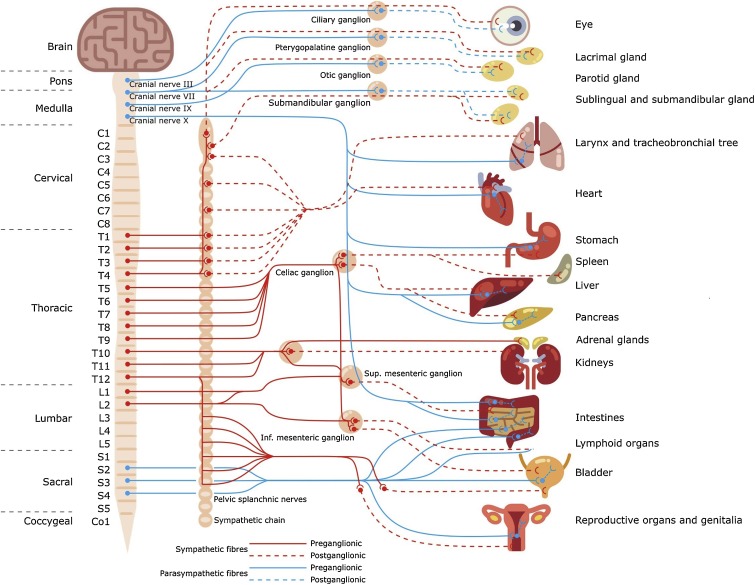
The – ‘Rest & Digest’ – Vagus nerve is the most important nerve you have. It is more than 10km long and forms the main part of the parasympathetic nervous system. It for instance controls the ‘resting phases’ of the heart and lungs. The vagus nerves are responsible for the lowering of the heart rate and in the lungs the vagus nerve causes bronchoconstriction to enable efficient oxygenation. A person usually dies quite quickly if the vagus nerve remains in full shutdown.
When the autonomic nervous system is working normally, the vagus nerve is speeding up the heart rate during inhalation and decreases heart rate during exhalation. This variation is critically important for optimal oxygenation. One traditional way to see this vagal tone is by measuring Heart Rate Variability (HRV) but for it to be accurate the measurement should be done for longer times and not by optical heart rate sensors which are inherently inaccurate. Currently, there are also many other indirect forms to quantify this oxygenation with wearable sports- and health devices.
Vagus Test
The Vagus ECG test is the first breathing based test for smartwatches that can make a quick and precise diagnosis of the second-to-second interaction between heart rate and breathing. Our algorithms can detect the timing and strength of every breath from the ECG data by using the Cardiac Brody Effect (1). The breathing data is then compared to pulse changes and from peak-to-peak timing correlations we calculate the Respiratory Sinus Arrhythmia (RSA). RSA is considered the best current scientific measurement of vagal tone = how well your ‘rest & digest’ nervous system is working. Based on our scientific research we have then, in addition to this RSA, developed a method to detect and diagnose the periodicity of heart rate increases and decreases in relation to each inhale and exhale (2). We call these cardiac/respiratory correlation values the Respiratory Sinus Arrhythmia Synchronization (RSAsync, pat.pend). The test lasts only 30 seconds and the user only needs to take 3 deep breaths.
NB: Atrial Fibrillation (AFib) automated detection. There is much reason to believe that the majority of the automated Atrial Fibrillation (AFib) detections in current ECG smartwatches are false positives for less than 65-year old users. There is not sufficient scientific research which would show that the benefits from such automated AFib detections in young people outweigh the adverse health effects from the excessive false positives. We have therefore decided not to provide or apply for medical AFib approval for the Vagus Health ECG smartwatch at this time. We strongly recommend consulting a cardiologist if the user suspects they have a repeating heart condition with AFib.
Recommended Reading
Professor Stephen Porges books about Polyvagal Theory. Dr. Porges is a Distinguished University Scientist at Indiana University where he directs the Trauma Research Center in the Kinsey Institute. In 1994 he proposed the Polyvagal Theory, a theory that links the evolution of the mammalian autonomic nervous system to social behavior and emphasizes the importance of the physiological state in the expression of behavioral problems and psychiatric disorders. There are several books published by Dr. Porges about the polyvagal theory and how ventral vagus nerve stimulation can help to alleviate symptoms in a number of diseases.
Professor Edward Bullmores, ‘The Inflamed Mind’: Cambridge University Professor Ed Bullmore is writing about how depression which will be the single biggest cause of disability worldwide in the next 20 years and how treatment for depression has not changed much in the last three decades. In his book, ‘The Inflamed Mind: A radical new approach to depression’, he reveals the breakthrough links found between depression and inflammation of the body and brain, representing a whole new way of looking at how mind, brain and body all work together. This book is a good description on how the vagus nerve, immune system and homeostasis are linked to depression and anxiety.
Professor Antonio Damasios books about how the brainstem formulate ‘will’.
Oliver Sacks ‘Awakenings’, 1990 edition. In the 1990 edition Oliver Sacks made a lot of additions to the original Awakenings book and many fine new conclusions. Awakenings is generally considered on of the best ‘patient observer’ book written in neurology.
Selected Science Papers
There are thousands of science papers published annually which discuss the vagus nerve and vagus stimulation so it is difficult to give a comprehensive list. Here are those used for our own vagal tone study presented in April 2019:
1) Assessment of cardiac preload and left ventricular function under increasing levels of positive end-expiratory pressure. Leucke, Thomas; Roth, Harry (1993). Intensive Care Medicine. 30 (1): 119–126.
2) Mechanism of decreased left ventricular stroke volume during inspiration in man. Pathophysiology and natural history. Authors: M. Karam, M.D., R. A. Wise et al.
3) Effect of respiration on cardiac filling at rest and during exercise in Fontan patients: A clinical and computational modeling study. IJC Heart & Vasculature, Volume 9, 7 December 2015, Pages 100-108 Authors: Alexander Van De Bruaenea
4) Respiratory change in ECG-wave amplitude is a reliable parameter to estimate intravascular volume status: Journal of Clin Monit Comput. Giraud R. Siegenthaler N. Morel DN,
5) Two Distinct Responses of Left Ventricular End-Diastolic Pressure to Leg-Raise Exercise in Euvolemic Patients with Exertional Dyspnea, Korean Circulatory Journal, May 2016. Authors: SeongIl Choi, MD1 , Jeung-Hun Shin, MD1, Whan-Cheol Park, MD1 , Soon-Gil Kim, MD1, Jinho Shin, MD2 , Young-Hyo Lim, MD2, and Yonggu Lee, MD3,
6) Cytokine-specific Neurograms in the Sensory Vagus Nerve. Bioelectron Med. 2016, Benjamin E Steinberg, Harold A Silverman, Sergio Robbiati, Manoj K Gunasekaran1, Téa Tsaava1, Emily . Battinelli1, Andrew Stiegler4, Chad E Bouton5, Sangeeta S Chavan1,†, Kevin J Tracey1,
7) Mechanisms and Therapeutic Relevance of Neuro-immune Communication, Immunity, June, 2017 Sangeeta S. Chavan,Valentin A. Pavlov and Kevin J. Tracey
8) The vagus nerve and the inflammatory reflex—linking immunity and metabolism. Nat Rev Endocrinol. 2012 December. Valentin A. Pavlov and Kevin J. Tracey
9) Theoretical Analysis of Intracavitary Blood Mass Influence on the Heart-Lead Relationship, 1956, By Daniel A. Brody, M.D.
10) The Brody effect and change of the volume of the heart. J. Electrocardiology 18, 1985, J. N. Amoore
11) The Brody Effect Revisited, Journal of Electrocardiology, October 1991, A. Van Oosterom, R. Plonsey.
12) Respiratory change in ECG-wave amplitude is a reliable parameter to estimate intravascular volume status, J. Clin Monit Comput (2013) 27:107–111, Raphael Giraud, Nils Siegenthaler, Denis R. Morel • Jacques-A Romand, Laurent Brochard • Karim Bendjelid
13) Respiratory sinus arrhythmia in humans: how breathing pattern modulates heart rate, 1981, Judith Ann Hirsch, Beverly Bishop.
14) Toward Understanding respiratory sinus arrythmia: Relations to cardiac vagal tone, evolution and biobehavioral functions. Biological Psychology 74, 2007. Paul Grossman, Edwin W. Taylor.
15) The Polyvagal Perspective, Bil Psychol Feb 2007 and several other papers and books by Stephen Porges on Respiratory Sinus Arrythmia (RSA) and the Polyvagal
Theory.
16) Accuracy of assessment of cardiac vagal tone by heart rate variability in normal subjects. Am J Cardiol 1991, Hayano J, Sakakibara Y. Yamada A, et al.
17) Respiratory modulation of cardiac vagal tone in Lyme disease. World J Cardiol, June 2014. Basant K. Puri, Musadiq Shah, Jean A. Monro, Michele C. Kingston, Peter OO Julu.
18) Anatomic connections of the diaphragm influence of respiration on the body system. Bordoni, B., & Zanier. (2013). Journal of Multidisciplinary Healthcare, 281.
19) Techniques of EMG signal analysis: detection, processing, classification and applications, Raez, Hussain & Mohd-Yasin, 2006
20) Physiology of the Autonomic Nervous System, Laurie Kelly McCorry, 2007
21) The Brody Effect to detect hypovolemia in clinical practice, R. Giraud et al, Critical Care, 2012
22) ‘Vagal Tone Diagnostics with hand-to-hand ECG, Gustaf Kranck et al, presented April 2019 at the Biofeedback Federation annual meeting in Wales.
Want to know more?
Sign up for our blogposts and updates
